Cosmetic clinics to assess mental health before offering Botox
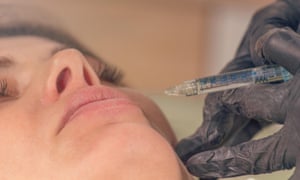
Cosmetic clinics will begin assessing patients’ suitability for Botox in an attempt to spot those whose desire to alter their appearance is due to mental health problems.
The Joint Council for Cosmetic Practitioners (JCCP), a trade body, has decided that member clinics will introduce new practices designed to protect the psychologically vulnerable. It has acted after the NHS’s top doctor claimed that the cosmetic industry was doing too little to stop those with body image obsessions undergoing potentially harmful treatments.
In future, clinic staff will be trained to understand the issues around people’s appearance and how to spot signs that a would-be customer may have a mental health problem. Anyone who appears vulnerable could be advised to seek help and directed to nearby NHS mental health services.
“Cosmetic firms bringing in tighter controls to protect young people’s mental health is a major step forward,” said Prof Stephen Powis, NHS England’s medical director.
However, he added, the new measures do not go far enough. “Voluntary steps on their own mean mental health too often will still be left in the hands of providers operating as a law unto themselves.
“Appearance is one of the things that matters most to young people, and the bombardment of idealised images and availability of quick-fix procedures is helping fuel a mental health and anxiety epidemic.”
There is concern that not all cosmetic firms belong to the JCCP and that they may not therefore implement the changes it has agreed.
Powis said anyone considering having Botox or other anti-ageing procedures in future should check whether the clinic belongs to the JCCP and that it has brought in the extra safety measures.
Simon Withey, a consultant plastic surgeon and chair of the Cosmetic Practice Standards Authority (CPSA), said: “We are grateful to NHS England, and its medical director, Stephen Powis, for adopting a firm stance on patient protection and highlighting the critical importance of considering the psychological welfare of patients engaging in aesthetic surgery and in non-surgical procedure.”
Bodies representing surgeons who perform invasive cosmetic treatment, including the British Association of Aesthetic and Plastic Surgeons, and the Royal College of Surgeons, are backing NHS England’s moves to make the industry more responsible.
The move follows the lead set by Superdrug, the high street beauty and pharmacy chain. It announced in January that it was improving its screening for mental health problems in those seeking to improve their appearance.
It planned to start using a questionnaire, intended to spot vulnerable patients, endorsed by the Body Dysmorphic Disorder Foundation. Body dysmorphic disorder is a condition in which sufferers obsess so much about what they perceive to be flaws in the way they look that they can become very distressed. About one in 50 people is believed to suffer from the condition.
Kitty Wallace, a trustee of the foundation, said: “We know that people with body dysmorphic disorder are more likely to turn to ‘quick-fix’ procedures that ultimately do not address or help the underlying psychological condition.”
Tom Madders, campaigns director at YoungMinds, said: “Young people who are struggling with their mental health often feel pressure around body image, so it’s good news that staff at cosmetic firms will receive training to spot the signs of poor mental health.
“But we also need wider action across society to help young people feel positive about who they are and how they look. The fashion, music and advertising industries should all be doing more to promote authentic and diverse body images.”